Rehabilitation Protocols: Time to Stop?
Physical therapy continues to apply rehabilitation techniques on a regular basis. I just conducted a little poll of my readers, and they mostly concur. Most people continue to adhere to protocol:
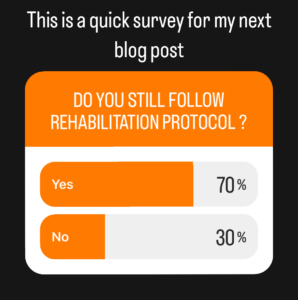
However, there has been a recent rise in criticism of these rules and individuals who adhere to them on social media. Even after graduating from college, students are refusing to follow standards.
Instead of following a piece of paper, we must utilize our minds.
Physiatrists shouldn’t use a recipe book.
Physical therapy is not a binary process. We must personalize our therapy strategy. I can at least somewhat comprehend and concur. We have devoted a lot of time and effort to our education on the workings of the human body as physical therapists (or other rehabilitation specialists). We’ve put many hours (and money…) into becoming physical therapists and become the best at what we do. Based on our experiences and the results of our patients, we have spent years honing our talents.
We need to be utilizing our minds and customizing programs for every individual. But if we apply rehabilitative methods appropriately, we can do this more effectively. To better understand how we should be employing rehabilitation protocols in our practices, it helps to break down precisely what they are and are not in physical therapy.
⇒Rehabilitation protocols are not recipes
First and foremost, rehabilitation protocols are not intended to be entire recipe manuals. This is where protocols may immobilize a physical therapist, leading them to believe that they can’t perform anything that isn’t clearly specified in the protocol.
A solid rehabilitation strategy should explicitly describe the objectives, precautions, and timetables for progressively applying stress to recovering tissue. These are founded on our knowledge of the fundamental science of the healing process. There is still a lot of gray space between what you SHOULD be doing and what you SHOULD NOT be doing.
Consider this a chance to personalize your recipe and create your own sandwich. You must toast the bread on both sides, but the amount of cheese you place between the pieces will vary depending on the patient, your training, and your expertise.
I often perform things with my patients that are not precisely specified in a protocol but that I know are in line with the protocol’s aims and precautions. Working the soft tissue of the trapezius following rotator cuff surgery is an excellent example. It is as integrating core exercise in the early stages of ACL recovery. Just because they aren’t explicitly included in the protocol doesn’t imply you can’t do them. Your program’s rehabilitation procedures are the cornerstone, and they should be altered depending on:
- Each person’s distinct objectives
- The particular injury or operation
- Any associated injuries, which are common
⇒Following an injury, rehabilitation protocols serve as guidelines
One widespread misperception about protocols is that they are specific regulations rather than suggestions. All of the nonoperative rehabilitation protocols that we have developed over the years are meant to guide you through the phases of rehabilitating a patient after an accident.
In reality, many do not even have fixed timeframes attached to them, but rather stages with progression requirements. For example, while rehabbing a Cricket player Kane Williamson forced out of IPL (2023) by knee injury. The following are some of the aims of each phase:
Phase 1: Promote healing by restoring range of motion and developing baseline strength and proprioception.
Phase 2: Continue range of motion while increasing strength and dynamic stability.
Phase 3: Apply stress to tissue gradually, then graduate to sport-specific dynamic exercises.
Phase 4: Return to sport progression.
Using the aforementioned stages as a reference, you may assess what is and is not acceptable for each phase. This is when your own tastes come into play. Postoperative care is different, and we’ll go over it in more detail later, but for nonoperative care, this is how you should employ a protocol. Nonoperative injuries may need limiting an exercise or activity for a period of time; nonetheless, nonoperative rehabilitation procedures are more frequently than not employed to break the rehab sequence into manageable pieces.
⇒Surgery Requires Rehabilitation
I believe in post-surgery rehabilitation procedures. Postoperative physical therapy requires rehabilitation methods. To help patients recover, post-surgery care guidelines must be established and conveyed. Surgeons may recommend going faster or slower depending on their expertise. Physical therapists must follow the surgeon’s instructions. They understand their procedure and your patient better than you. Protocols protect, heal, and load damaged tissues after surgery. Without a process, you’re unlikely to return the individual promptly and securely. At 6 weeks after an anterior labral surgery, too much shoulder range of motion may be harmful. A well-planned postoperative rehabilitation strategy will help the patient succeed.
⇒Rehabilitation Protocols: Time to Stop?
I don’t believe so; in fact, I am a firm believer in rehab techniques when they are implemented effectively. I believe it is incredibly naïve to disregard procedures as harmful to our profession or as something we are above utilizing.
A protocol, on the other hand, merely specifies what you may and cannot do. What you “can” accomplish is not limited to what is specified in the protocol. Consider these recommendations to ensure that you are not moving too slowly or too quickly. A protocol, in reality, does not cover every therapy and exercise that should be included. This is where your knowledge and expertise come in handy. You must consider what alternative treatments you may safely undertake to assist the patient, while also determining if the selected action fits safely within the protocol constraints.
We should not blindly follow a rehabilitation regimen; this is not “skilled” physical therapy. However, we must recognise the timetables that are often connected with procedures and healing tissues.
The truly expert doctor recognizes this and integrates rehabilitation procedure recommendations with their wide knowledge and therapy choices.




